Defining True Resistance
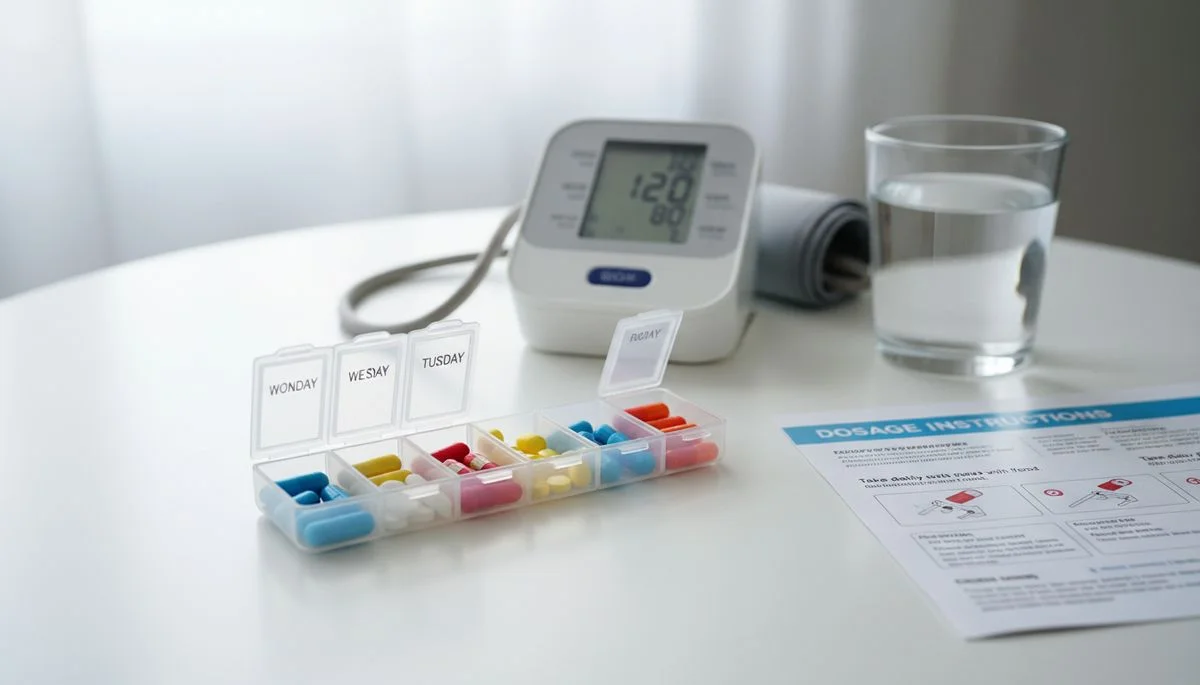
Resistant hypertension is defined as blood pressure above 130/80 mmHg despite optimal doses of three antihypertensive medications from different classes, one of which is a diuretic. It's important to distinguish true resistant hypertension from "pseudo-resistant" hypertension, which is far more common. Pseudo-resistance results from: medication non-adherence (the most common cause), white-coat hypertension (blood pressure is truly controlled but appears high in clinical settings), suboptimal medication regimens (not including a diuretic, inadequate doses, or drug interactions), poor blood pressure measurement technique, and lifestyle factors (high sodium intake, excessive alcohol, sleep apnea).
Ruling Out Secondary Causes
Before accepting a diagnosis of resistant hypertension, physicians should systematically investigate secondary (treatable) causes, which account for 20–40% of truly resistant cases. The most important is primary aldosteronism — excess production of the hormone aldosterone by the adrenal glands, causing sodium retention and treatment-resistant hypertension. Other causes include renal artery stenosis, obstructive sleep apnea (found in over 80% of resistant hypertension patients), chronic kidney disease, thyroid dysfunction, pheochromocytoma (rare adrenal tumor), and certain medications.
Advanced Treatment Options
For patients with confirmed resistant hypertension after addressing pseudo-resistance and secondary causes, treatment options include: adding a fourth medication (typically spironolactone, an aldosterone antagonist, which is remarkably effective for primary aldosteronism-related resistance); renal denervation — a minimally invasive catheter procedure that disrupts the sympathetic nerves supplying the kidneys, recently approved by the FDA; intensive lifestyle modification with particular focus on sodium restriction, weight loss, and aerobic exercise; and referral to a hypertension specialist.
The Importance of Meticulous Home Monitoring
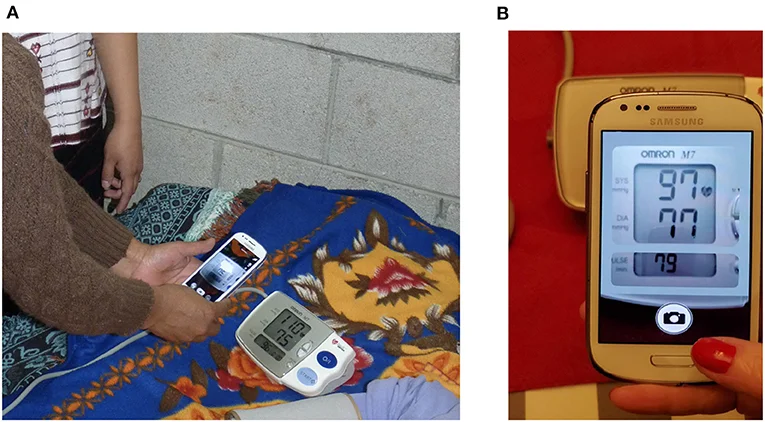
In resistant hypertension, the distinction between true resistance and pseudo-resistance depends critically on reliable blood pressure data. Twice-daily home monitoring with a validated device, using perfect technique, over at least 2–4 weeks provides the quality data needed to guide treatment decisions. Ambulatory blood pressure monitoring (ABPM) — a device worn for 24 hours that measures pressure every 20–30 minutes — is the gold standard for distinguishing white-coat from true resistant hypertension and is often ordered before escalating treatment.