What Does a Blood Pressure Reading Actually Mean?
When your blood pressure monitor shows "127/81," what exactly are you looking at? Blood pressure is measured as two numbers separated by a slash. The top number is systolic pressure — the force your heart exerts when it beats and pumps blood. The bottom number is diastolic pressure — the pressure in your arteries between beats, when your heart is at rest.
Both numbers matter. Isolated high systolic pressure (called isolated systolic hypertension) is extremely common in people over 60 and carries significant cardiovascular risk even if diastolic pressure is normal.
The AHA Blood Pressure Categories
The American Heart Association classifies blood pressure into five categories:
- Normal: Less than 120/80 mmHg — your cardiovascular risk is low. Continue healthy habits.
- Elevated: 120–129 / less than 80 mmHg — blood pressure is creeping up. Lifestyle changes can prevent progression to hypertension.
- High Blood Pressure Stage 1: 130–139 / 80–89 mmHg — your doctor will likely recommend lifestyle changes and may consider medication depending on your overall risk.
- High Blood Pressure Stage 2: 140 or higher / 90 or higher mmHg — medication is typically recommended alongside lifestyle changes.
- Hypertensive Crisis: Over 180/120 mmHg — seek emergency medical care immediately.
What's "Normal" Changes After Age 65
For decades, doctors considered 150/90 mmHg acceptable for older adults. The landmark SPRINT trial changed this. It showed that treating seniors to a systolic target below 120 mmHg reduced cardiovascular events by 25% and death by 27% compared to a target of 140. However, treatment targets must be individualized. Seniors with frailty, orthostatic hypotension, or certain conditions may benefit from higher targets to prevent dangerous falls from over-treatment.
The most current guidance from the American College of Cardiology suggests a target below 130/80 mmHg for most older adults who can tolerate it safely.
Pulse Pressure: The Number Most People Ignore
Pulse pressure is the difference between systolic and diastolic readings. A reading of 130/80 gives a pulse pressure of 50. Normal pulse pressure is 40–60 mmHg. A widening pulse pressure (above 60) in older adults is an important risk marker for cardiovascular disease, reflecting arterial stiffness. If your pulse pressure is consistently above 60, discuss it with your physician.
Heart Rate vs. Blood Pressure
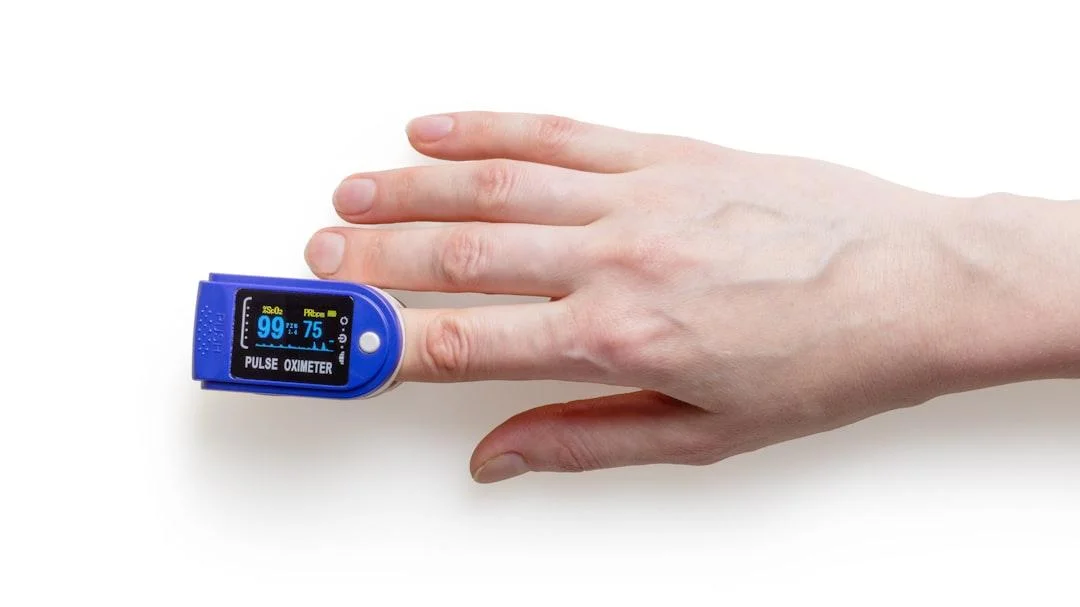
Your blood pressure monitor likely shows a third number: pulse (or heart rate). Blood pressure and heart rate are related but not the same. A high heart rate doesn't necessarily mean high blood pressure, and vice versa. A resting heart rate of 60–100 beats per minute is considered normal. However, a consistently elevated resting heart rate above 80 bpm — even with normal blood pressure — is associated with higher cardiovascular risk.
White-Coat Hypertension: Why Doctor Readings Are Often Higher
Studies show that up to 30% of people diagnosed with hypertension in a clinical setting have normal blood pressure at home — a phenomenon called white-coat hypertension. The anxiety and stress of a medical appointment triggers a temporary blood pressure increase. This is why home monitoring is so important. If your home readings are consistently below 135/85, but your doctor's office readings are above 140/90, mention this discrepancy to your physician.
Masked Hypertension: The Hidden Danger
The opposite also occurs: some people have normal blood pressure at the doctor but elevated readings at home or during daily activity. Called masked hypertension, this affects roughly 15% of adults and significantly increases cardiovascular risk. Regular home monitoring is the only way to detect it.
When to Measure for the Most Accurate Reading
To get the most accurate home readings: sit quietly for 5 minutes before measuring; don't exercise, smoke, or drink caffeine within 30 minutes; sit with your back supported and feet flat on the floor; keep your arm at heart level; take two readings one minute apart and average them; record readings in the morning (before medication) and evening.
Understanding Your Trend, Not Just One Reading
A single reading tells you very little. Blood pressure naturally fluctuates throughout the day — it's lowest during sleep, rises sharply upon waking, peaks in the mid-morning, dips after lunch, and rises again in the late afternoon. What matters is the pattern over days and weeks. Apps like SnapVitals automatically track and display your trend, making it easy to see whether your lifestyle changes and medication are working.