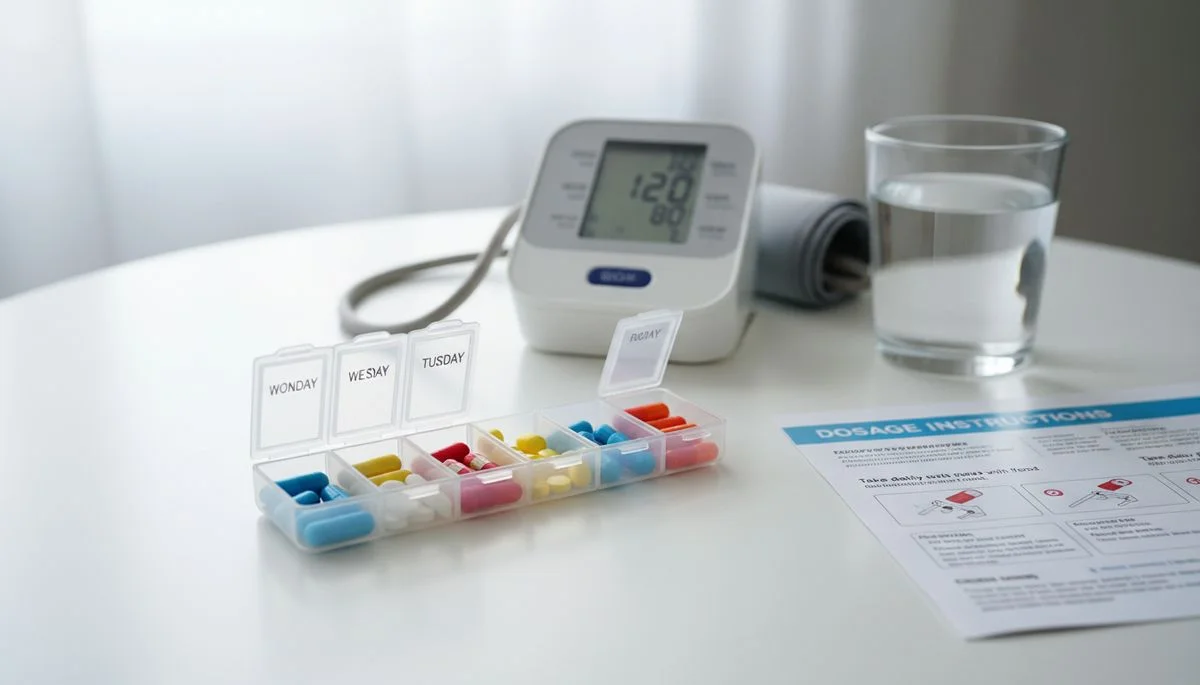
Why Medication Management Is Different for Seniors
Blood pressure medications that work perfectly at age 50 may behave differently at age 75. Older adults experience changes in kidney and liver function, altered drug distribution due to shifts in body composition, and increased sensitivity to medications affecting blood pressure and heart rate. Polypharmacy — taking multiple medications simultaneously — is extremely common in seniors and creates complex interaction risks. This makes close collaboration with your doctor, pharmacist, and regular blood pressure monitoring especially important.
The Main Classes of Blood Pressure Medications
ACE Inhibitors (lisinopril, enalapril, ramipril): These block the production of angiotensin II, a hormone that narrows blood vessels. They're particularly beneficial for seniors with diabetes or kidney disease. The most common side effect is a dry, persistent cough in 10–15% of users. If bothersome, ARBs are an effective alternative without this side effect.
ARBs (losartan, valsartan, olmesartan): Similar to ACE inhibitors but block angiotensin II at its receptor rather than preventing its production. Generally very well-tolerated in older adults, with a lower side-effect profile than ACE inhibitors. Both ACE inhibitors and ARBs protect the kidneys and are preferred first-line agents in seniors with diabetes.
Calcium Channel Blockers (amlodipine, diltiazem, verapamil): These relax blood vessel walls by blocking calcium from entering cells. Amlodipine is one of the most commonly prescribed blood pressure medications for seniors and is generally well-tolerated. Non-dihydropyridine CCBs (diltiazem, verapamil) also slow heart rate and must be used cautiously with other heart rate-lowering medications.
Diuretics (hydrochlorothiazide, chlorthalidone, furosemide): Often called "water pills," diuretics help kidneys eliminate excess sodium and water, reducing blood volume and pressure. They're often the first-line choice for isolated systolic hypertension in seniors. Side effects can include electrolyte imbalances (particularly low potassium), increased urination, and rarely gout.
Beta-Blockers (metoprolol, atenolol, carvedilol): Reduce heart rate and the force of contractions. Now considered second-line for hypertension alone but first-line for seniors with concurrent heart failure or coronary artery disease. Side effects include fatigue, cold extremities, and sexual dysfunction. Never stop beta-blockers abruptly — gradual tapering is required.
Common Side Effects in Seniors to Watch For
Orthostatic hypotension — a sudden drop in blood pressure when standing — is particularly dangerous in seniors, increasing fall risk. It's most common with alpha-blockers, diuretics, and medications taken in higher doses. Rise slowly from sitting or lying positions, especially in the morning. If you feel lightheaded upon standing, sit back down immediately.
First-dose hypotension: some medications cause a larger-than-expected drop with the first dose. Starting at a lower dose and taking the first dose at bedtime reduces this risk.
Medication Timing Strategies
The timing of blood pressure medication can be as important as the dose. Several studies suggest that taking at least one antihypertensive medication at bedtime (rather than all in the morning) may provide better 24-hour blood pressure control and significantly reduce cardiovascular event risk. Discuss this with your doctor — medication timing should be individualized based on your blood pressure pattern, which home monitoring can reveal.
The Role of Home Monitoring in Medication Management
Regular home monitoring is essential when taking blood pressure medications. It helps detect if medication is working, if dosing needs adjustment, if side effects are causing over- or under-treatment, and if your pattern changes over time. Bring your home monitoring log — or a SnapVitals PDF report — to every doctor's appointment. Your physician can make much better informed decisions with 2–4 weeks of twice-daily readings than with a single office measurement.
Never Adjust Medications Without Guidance
Never stop, skip, or change the dose of blood pressure medications on your own. Stopping some medications abruptly — especially beta-blockers and clonidine — can cause a dangerous rebound rise in blood pressure. If you're experiencing side effects or your readings are very low, contact your doctor before making any changes to your regimen. Keep an up-to-date medication list with doses and timing, and review it with your pharmacist annually to check for interactions.