The Nocturnal Blood Pressure Dip
In healthy adults, blood pressure follows a predictable 24-hour cycle. During sleep, it naturally decreases by 10–20% — a pattern called nocturnal dipping. This nightly rest period is essential for cardiovascular recovery. People who fail to experience this dip (called "non-dippers") have significantly higher rates of heart attack, stroke, and kidney disease — even if their daytime blood pressure is normal.
Poor sleep quality — whether from insomnia, frequent waking, or sleep apnea — disrupts this restorative dip. The consequence is that the cardiovascular system never fully rests, contributing to cumulative damage over years and decades.
Sleep Apnea: The Silent Blood Pressure Thief
Obstructive sleep apnea (OSA) affects an estimated 20–30% of older adults, and many cases go undiagnosed. During apnea episodes, the airway collapses repeatedly during sleep, causing oxygen levels to drop and the body to release stress hormones that spike blood pressure — sometimes hundreds of times per night. Studies show that untreated sleep apnea increases the risk of treatment-resistant hypertension by 200–300%. Signs include loud snoring, witnessed breathing pauses, morning headaches, and daytime sleepiness. A sleep study can confirm the diagnosis, and CPAP therapy is highly effective at both treating the apnea and lowering blood pressure.
How Many Hours of Sleep Do Seniors Need?
While older adults often experience changes in sleep architecture — less deep sleep, more frequent awakenings — the need for sleep doesn't decrease with age. Most seniors need 7–8 hours of actual sleep per night. Studies consistently show that sleeping fewer than 6 hours is associated with significantly higher blood pressure and cardiovascular event risk. Spending 8 hours in bed but sleeping for only 5–6 hours still carries health risks.
8 Evidence-Based Sleep Hygiene Tips
Keep a consistent schedule: Go to bed and wake at the same time every day, including weekends. This regulates your circadian rhythm, improving both sleep quality and blood pressure regulation.
Keep the bedroom cool: A room temperature of 65–68°F (18–20°C) is optimal for sleep. Body temperature naturally drops during sleep, and a cool room supports this process.
Eliminate blue light exposure: Screen light from phones, tablets, and TVs suppresses melatonin production. Avoid screens for at least 60 minutes before bed. If necessary, use blue light glasses or night mode settings.
Avoid caffeine after 2 PM: Caffeine has a half-life of 5–6 hours, meaning half of a 3 PM coffee is still in your system at 8 PM. Even people who "sleep fine" with evening caffeine typically experience reduced sleep quality and higher nighttime blood pressure.
Limit evening fluids: Waking to urinate disrupts sleep architecture. Reduce fluid intake in the 2 hours before bed, and empty your bladder immediately before sleeping.
Use your bed only for sleep: Associating the bed with activity (reading, watching TV, worrying) weakens the mental cue for sleep. Train your brain to connect bed with sleep only.
Address nocturia: Frequently waking to urinate is extremely common in older adults and significantly disrupts sleep. Discuss this with your doctor — treatment options include medication adjustments, pelvic floor exercises, and dietary changes.
Consider melatonin: Low-dose melatonin (0.5–1 mg) taken 30–60 minutes before bed can help seniors with circadian rhythm disruption. Unlike prescription sleep aids, low-dose melatonin is non-addictive and doesn't cause next-day grogginess.
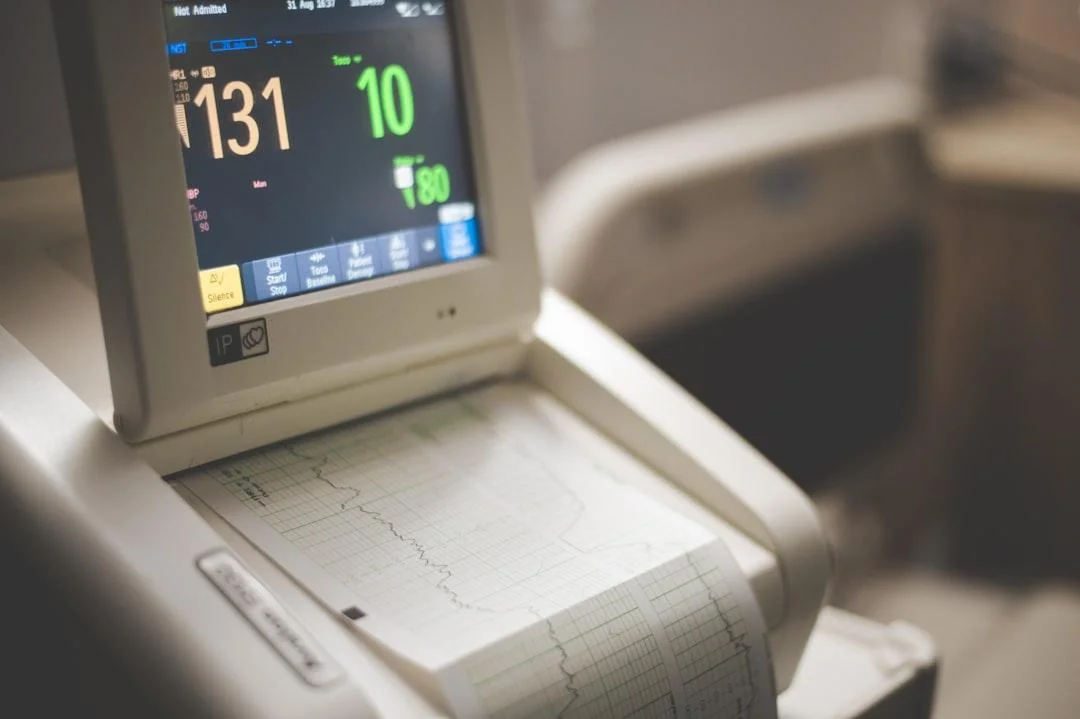
Monitoring Blood Pressure Around Sleep
Measuring your blood pressure first thing in the morning — before getting out of bed and before taking medications — gives you your post-sleep reading. A reading above 130/80 first thing in the morning suggests your blood pressure may not be dipping adequately during sleep. If you notice a pattern of high morning readings alongside daytime fatigue, snoring, or restless sleep, discuss sleep apnea screening with your physician.