The Disparity in Numbers
The statistics are stark: African Americans have the highest rates of hypertension in the world. Approximately 60% of Black adults in the United States have hypertension, compared to 47% of white adults. The condition develops earlier (often before age 40), is more severe (higher average blood pressures), is less well-controlled despite treatment, and produces disproportionately higher rates of end-organ damage — including stroke rates 50% higher, kidney failure rates 3 times higher, and heart failure rates nearly twice as high as in white Americans.
Biological and Social Factors
The causes are multifactorial and include both biological and social determinants. Biologically, Black Americans have greater salt sensitivity on average — the kidneys retain more sodium per unit of dietary intake, producing larger blood pressure increases from the same sodium exposure. Lower renin levels mean that RAAS-targeting medications (ACE inhibitors, ARBs) are less effective as single agents. Socially, decades of research document the cardiovascular impact of chronic stress from racial discrimination, housing insecurity, limited healthcare access, and economic inequality — creating a persistent physiological stress burden that drives autonomic hypertension.
Treatment Differences That Matter
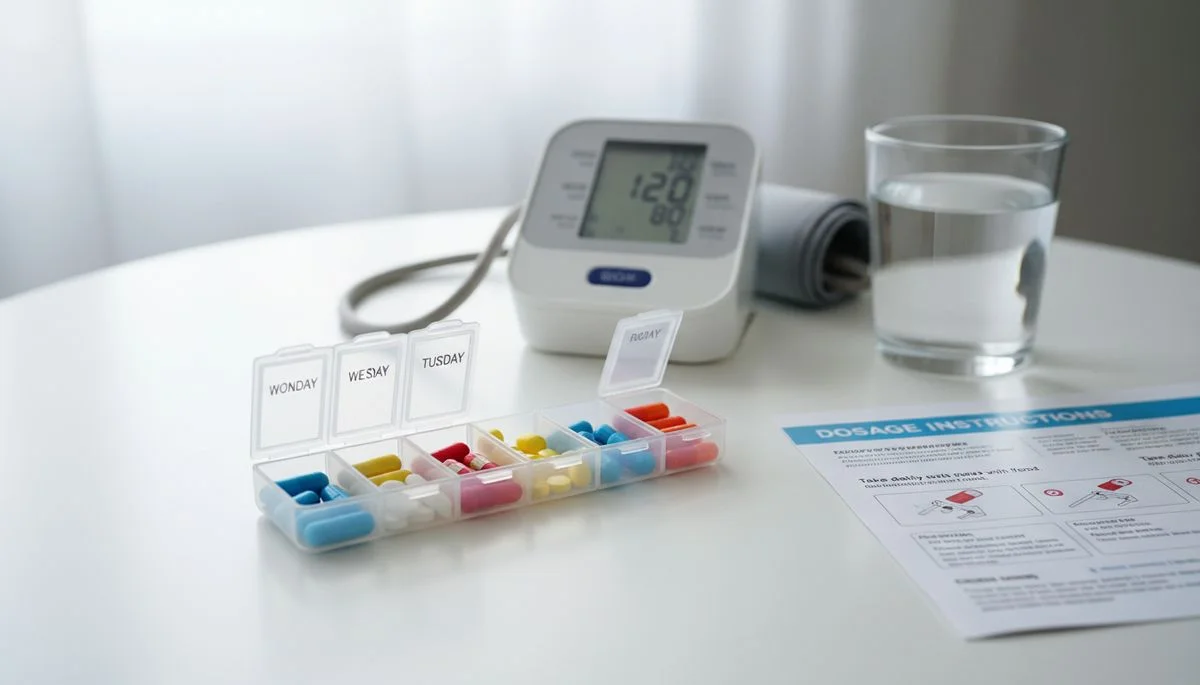
Treatment guidelines now specifically address racial pharmacological differences. For Black patients with hypertension without diabetes or kidney disease, thiazide diuretics and calcium channel blockers as initial therapy are generally more effective than ACE inhibitors or ARBs used alone. Combination therapy typically produces better results than monotherapy. Achieving blood pressure below 130/80 mmHg is especially important given the higher complication rates — even small reductions produce proportionally large risk reductions in this high-risk population.
Community-Based Solutions and Self-Advocacy
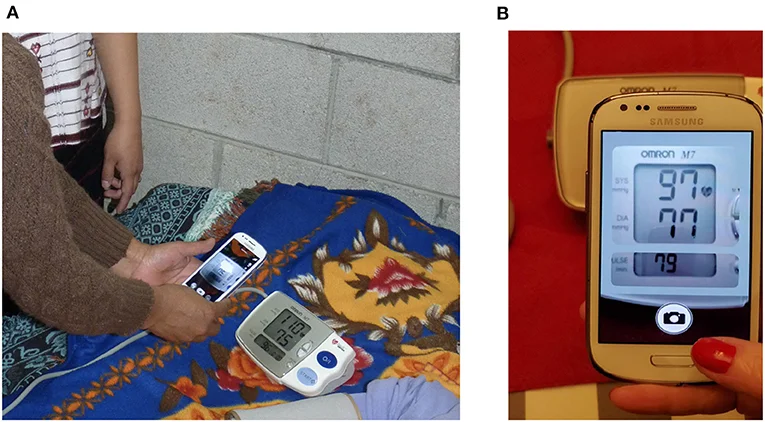
Community health worker programs, barbershop-based blood pressure programs (which have shown remarkable success in Black communities), faith community health initiatives, and culturally tailored home monitoring programs have demonstrated significantly better blood pressure control outcomes than standard care in Black communities. Home monitoring — removing white-coat effects and providing consistent data — is particularly valuable. Self-advocacy through regular monitoring, bringing printed blood pressure logs to appointments, and actively participating in treatment decisions all improve outcomes in a healthcare system that has historically underserved Black patients.